Huttons CBD
What is the Endocannabinoid System?
The endocannabinoid system (also known as the ECS) is a complex cell signalling system in the human body, discovered in the early 1990s by scientists researching cannabinoids. Cannabinoids are compounds naturally occurring in cannabis plants; CBD is one commonly known cannabinoid.
Experts are still trying to understand the endocannabinoid system fully. But we know it plays a role in regulating a range of functions and processes, including:
- sleep
- mood
- appetite
- memory
- anxiety
- stress
- motivation
- pain
- inflammation
- energy
The ECS exists and is active in your body regardless if you don’t use cannabinoids.
What is the ECS?
The ECS involves three core components: endocannabinoids, receptors, and enzymes.
Endocannabinoids
Endocannabinoids are molecules made by your body. They’re similar to cannabinoids, but your body produces them. These help keep internal functions running smoothly. Your body produces them as needed.
Experts have identified two key endocannabinoids so far:
- anandamide (AEA)
- 2-arachidonoylglyerol (2-AG)
Endocannabinoid Receptors
These receptors are found throughout your body. Endocannabinoids bind to them in order to signal that the ECS needs to take action.
There are two main endocannabinoid receptors:
- CB1 receptors, which are mostly found in the central nervous system
- CB2 receptors, which are mostly found in your peripheral nervous system, especially immune cells
Endocannabinoids can bind to either receptor. The effects that result depend on where the receptor is located and which endocannabinoid it binds to.
Enzymes
Enzymes in the body break down endocannabinoids once they’ve carried out their function.
There are two main enzymes responsible for this:
- fatty acid amide hydrolase, which breaks down AEA
- monoacylglycerol acid lipase, which typically breaks down 2-AG
How does it work?
The ECS is a complicated and relatively new field, and scientists haven’t yet determined exactly how it works or all of its potential functions.
Research so far has linked the ECS to these processes:
- appetite and digestion
- bone remodelling and growth
- cardiovascular system function
- chronic pain
- inflammation
- learning and memory
- liver function
- metabolism
- mood
- motor control
- muscle formation
- reproductive system function
- sleep
- skin and nerve function
- stress
These functions all contribute to homeostasis, which refers to the stability of your internal environment. To reach homeostasis, our bodily systems must find a balance. An example could be; an athlete applying more significant stress to their body, leading to pain and inflammation. This sends homeostasis out of balance; the endocannabinoid system then tries to restore balance to the body by helping to manage and reduce the pain and inflammation so that the body can return to ‘normal’. This is reaching homeostasis.
Today, some experts believe maintaining homeostasis is the primary role of the ECS.
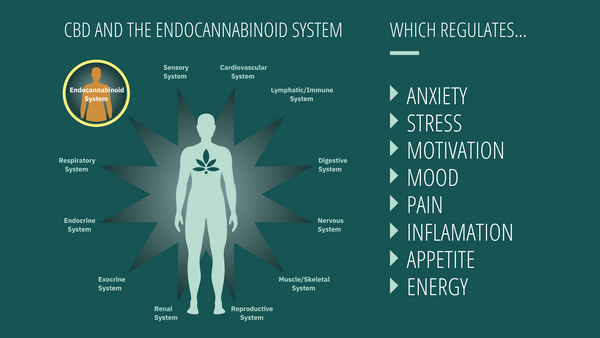
How does CBD interact with the ECS?
Due to a lack of research, experts aren’t sure yet exactly how CBD interacts with the ECS. But they have discovered that it doesn’t bind to CB1 or CB2 receptors like endocannabinoids.
One theory suggests that CBD works by preventing endocannabinoids from being broken down by enzymes – this allows them to have more of an effect on your body. Another theory suggests that CBD binds to a receptor that hasn’t been discovered yet. This is entirely possible as ECS research is so new.
Another increasingly popular theory is that of Clinical Endocannabinoid Deficiency (CECD); this theory suggests that low endocannabinoid levels could contribute to the cause of some chronic conditions such as fibromyalgia, migraines, ME, and IBS. None of these conditions has a clear underlying cause, and many anecdotal reports suggest that CBD and other cannabinoids positively affect managing these conditions.
If CBD does play any role in these conditions, targeting the ECS or endocannabinoid production could be the missing key to treatment, but more research is needed.